Cervical cancer begins with a persistent high-risk HPV infection that causes gradual changes in the normal cervical cells over 10–15 years.
These changes can be detected and treated early—long before cancer develops—especially with timely screening guided by a cervical cancer doctor, like Dr Joydeep Ghosh.
Here’s what most people don’t realise: this is one of the few cancers where your body gives you time. The risk isn’t speed—it’s silence. And silence is exactly why screening matters.
What causes cervical cancer? (Quick Overview)
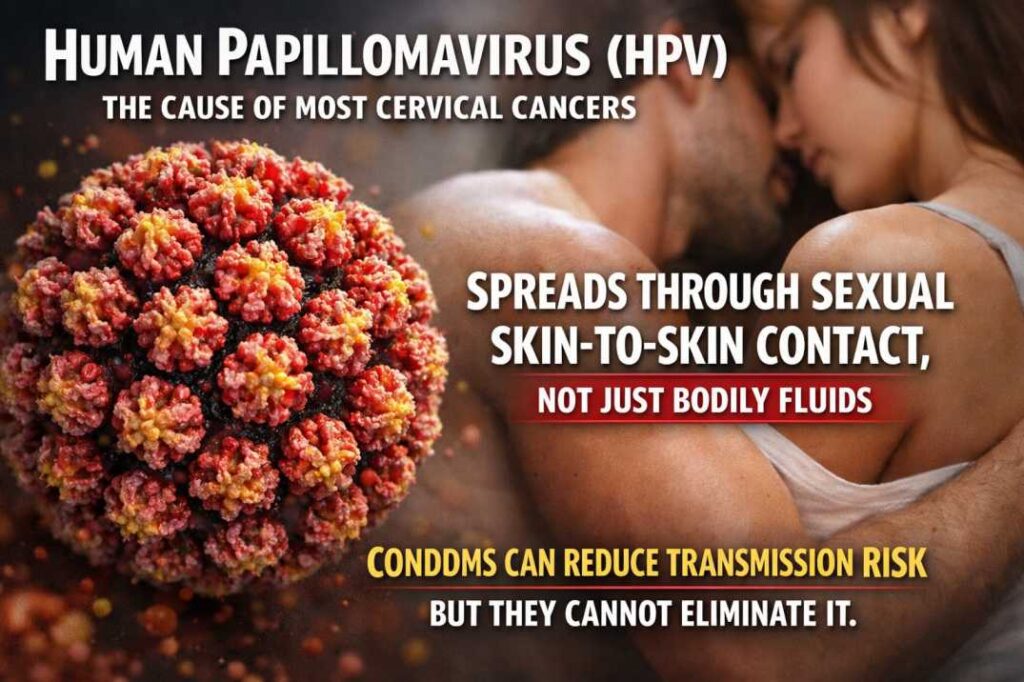
Cervical cancer is primarily caused by a persistent infection with high-risk types of human papillomavirus (HPV). While most HPV infections clear naturally within 1–2 years, long-lasting infections can trigger abnormal cervical cell changes over time. Notably, HPV types 16 and 18 alone are responsible for about 70% of cervical cancer cases worldwide. [Source]

Quick take: the “HPV → changes → cancer” timeline in one minute
HPV can lead to cervical cancer only when the infection persists and causes gradual changes in cervical cells. Most infections clear naturally, but some remain and progress from normal cells to precancer and eventually cancer if untreated.
Why this matters: cervical cancer usually develops slowly
Cervical cancer develops over years, not months—giving multiple chances to detect and treat early changes through regular cervical cancer screening. This makes it one of the most preventable cancers when screening is done on time.
What is HPV, and why does it target the cervix
HPV (human papillomavirus) is a common virus that spreads through skin contact and can infect cervical cells. In some cases, it causes long-term cellular changes that may lead to cancer if not detected early.
High-risk vs low-risk HPV: what’s the difference?
- Low-risk HPV: May cause warts but not cancer
- High-risk HPV: Can lead to cancer over time
Does HPV always cause cancer?
No. Most cases of HPV infection in women clear naturally within 1–2 years. HPV infection isn’t cancer. It becomes a risk only when high-risk HPV lingers over time.
Many women wonder Can I get pregnant with cervical cancer?’
Dr Joydeep Ghosh offers clarity through his video: Cervical Cancer হলে কি Pregnancy সম্ভব? Can You Get Pregnant with Cervical Cancer? Dr. Joydeep Ghosh
Cervical cancer’s “origin story”: from normal cells to pre-cancer
Cervical cancer develops through gradual stages, starting from HPV infection to precancerous changes and eventually cancer, giving multiple opportunities for early detection and prevention.
Step 1: HPV infection (often no symptoms)
HPV infection usually occurs without any symptoms, meaning most people don’t realise they have it while the virus begins affecting cervical cells.
Step 2: Persistent infection (when HPV doesn’t clear)
In some women, persistent HPV infection happens when the virus stays in the body over time, increasing the risk of cellular changes that may lead to precancer if not monitored.
Step 3: Precancerous changes (cervical dysplasia / CIN)
These early changes, called cervical dysplasia (also called precancerous cervical changes), are not cancer, but they are the stage where treatment works best.
Step 4: Cancer (when changes are missed for years)
If these changes go undetected and untreated, they can slowly progress into cancer.
(Special Mention)
[Source].
How long does it take for HPV to turn into cervical cancer?
It typically takes 10–15 years for HPV-related changes to become cancer, which is why timely screening is highly effective.
Typical timeframes (why screening works so well)
| Stage | Timeframe |
| HPV infection | Immediate |
| Persistent infection | 1–2 years |
| Precancer (CIN) | 3–10 years |
| Cancer | 10–15 years |
Why cervical cancer is often missed early
Cervical cancer is often missed early because it usually causes no symptoms in its initial stages and develops slowly, often over 15–20 years.
Early detection depends on regular Pap or HPV screening, which many women miss due to low awareness, stigma, or limited access to healthcare.
What makes cervical cancer progression more likely (risk factors)
- Smoking
- Low immunity
- Multiple HPV exposures
- Skipping regular screening
What are CIN, LSIL, and HSIL (and why do these terms show up in reports)
CIN (cervical intraepithelial neoplasia) is graded as:
- CIN 1: Mild changes
- CIN 2: Moderate changes
- CIN 3: Severe changes
LSIL vs HSIL (High-Grade Squamous Intraepithelial Lesion): what “low-grade” and “high-grade” usually mean
| Term | Meaning |
| LSIL | Low-grade changes, often temporary |
| HSIL | High-grade changes, higher cancer risk |
Early warning signs: when symptoms show up (and when they don’t)
Early cervical cancer typically shows no symptoms. That makes regular Pap smears and HPV tests vital.
When Symptoms Show Up
- Abnormal Vaginal Bleeding: Bleeding between periods, heavier/longer periods, or bleeding after intercourse.
- Postmenopausal Bleeding: Any bleeding occurring after menopause should be investigated.
- Unusual Vaginal Discharge: Watery, bloody, pale, or foul-smelling discharge.
- Pain During Sex: Discomfort or sharp pain during intercourse (dyspareunia).
- Pelvic/Lower Back Pain: Unexplained, persistent discomfort not related to a menstrual cycle
When symptoms do not show (the “silent” phase)
- Early-stage cervical cancer (Stage 1) and precancerous changes often cause no pain or visible symptoms
- HPV-related changes occur at a microscopic level, so you may feel completely normal. These early changes are only detectable through screening (Pap smear or HPV test).
This “silent phase” can last for years, which is why many cases go unnoticed without regular testing
When to seek immediate medical advice
- Persistent bleeding between periods, after sex, or after menopause
- Unusual vaginal discharge that does not resolve
- Ongoing pelvic pain or lower back pain that does not improve
These may be cervical cancer symptoms and should be evaluated early.
Why do many people have no cervical cancer symptoms in the early stages
Simply, because abnormal cells remain confined to the surface of the cervix and have not invaded deeper tissues or caused pain.
How to catch it early: cervical screening tests explained
- Pap smear
The Pap smear test detects early abnormal changes in cervical cells and is recommended for women starting in their 20s as part of routine screening to prevent cervical cancer.
- HPV test
The HPV test identifies high-risk virus types that can cause cervical cancer, often detecting risk earlier than cell changes appear, making it a powerful tool for early prevention.
- VIA test
The VIA test (visual inspection with acetic acid) is a simple screening method that highlights visible cervical changes using acetic acid and is widely used in public health settings for quick, low-cost detection.
Which test is “best” — and what doctors decide based on
| Test | Detects | Best for |
| Pap smear | Cell changes | Routine screening |
| HPV test | Virus presence | Early detection |
| VIA | Visible changes | Public health use |
Dr Joydeep Ghosh, a qualified cervical cancer doctor in Kolkata, helps patients decide the most suitable test based on their age, history, and risk profile.
If your screening is abnormal, what happens next
- Colposcopy
A colposcopy test is a detailed examination of the cervix using magnification to closely assess abnormal areas. It helps doctors decide if further testing or treatment is needed.
- Biopsy
A biopsy (the gold standard for diagnosing cancer) involves taking a small tissue sample from the cervix. It helps to confirm whether abnormal cells are precancerous or cancerous and guides the next steps in treatment.
Treating precancer: how doctors stop cancer before it starts
- Removal of abnormal cells
- Short, targeted procedures
- High success rates when detected early
How to prevent HPV-related cervical changes
HPV-related cervical cancer is largely preventable with HPV vaccination and regular screening.
HPV vaccine: who should take it and when
Recommended for individuals aged 9 to 45 years to protect against cancers caused by human papillomavirus (HPV).
- Ideal age: 11–12 years (can start as early as 9)
- Catch-up vaccination: Everyone up to age 26 (if not vaccinated earlier)
- Adults (27–45)
Safer-sex basics that actually reduce HPV spread
- Use protection
- Limit multiple partners
- Stay consistent with screening
Why smoking and low immunity matter more than people think
Smoking weakens the body’s ability to clear HPV, increasing the risk of long-term infection and progression.
When should you start screening (and how often)
| Age | Recommendation |
| 21–29 | Pap smear every 3 years |
| 30–65 | Pap + HPV co-testing every 5 years |
What to expect?
- Takes 5–10 minutes
- Mild discomfort, not pain
- No hospital stay needed
Kolkata section: where to get screened and what to ask before booking
Questions to ask
- Do you offer Pap, HPV, or co-testing?
- What is the reporting time?
- Is follow-up support available?
How to plan your appointment
- Avoid periods during the test
- Avoid intercourse 24 hours before
- Follow pre-test instructions carefully
Consult Dr Joydeep Ghosh, a trusted cervical cancer doctor in Kolkata, to guide you clearly.
Myths vs facts (quick clarity on common confusion)
“HPV means my partner cheated”
False. HPV can remain inactive for years before detection.
“If I feel fine, I don’t need screening”
Incorrect. Early stages usually have no symptoms.
“The HPV vaccine is only for teens”
Not true. Adults can benefit as well.
Final Verdict: The real win is catching cervical cancer early
- Cervical cancer is not sudden—it’s a slow, preventable process.
- HPV may start the chain, but timely screening breaks it.
- The earlier you act, the simpler the treatment and the better the outcome.
If you’re due for screening or unsure where to start, speak to Dr Joydeep Ghosh, a leading medical oncologist and cervical cancer doctor in Kolkata.
Book your private session today.
People Also Ask
Can HPV go away on its own?
Yes. Most infections clear naturally within 1–2 years.
Is cervical screening painful?
No. It may feel slightly uncomfortable, but it is quick.
What does it mean to be HPV positive with a normal Pap test?
It means the virus is present, but no abnormal cell changes are detected yet. Regular follow-up is important.
How accurate are Pap smear and HPV tests?
Both are highly reliable when performed correctly and regularly.
Is screening still needed after HPV vaccination?
Yes. The vaccine does not cover all high-risk HPV types.